Most people assume anxiety is something younger generations deal with. The racing thoughts before a job interview, the social nerves, the overthinking at 2 a.m. But anxiety doesn’t check out when a person turns 65. According to a 2024 systematic review published in the Journal of General and Family Medicine, nearly 28% of older adults worldwide experience clinically significant anxiety symptoms. That’s more than one in four seniors.
And here’s the part that should concern every family: only about one-third of older adults with generalized anxiety disorder receive any kind of treatment, according to research published in PMC’s psychiatric literature. Two-thirds are managing something very real, and very disruptive, completely alone.
This guide is for families, caregivers, and older adults themselves who want to understand what severe anxiety actually looks like in aging adults, why it so often gets missed, and what genuinely helps.
Why Anxiety Looks Different in Seniors
When most people think of anxiety, they picture someone wringing their hands or having a panic attack. In older adults, it usually looks nothing like that.
Anxiety in seniors tends to show up as physical complaints. Fatigue that doesn’t get better with rest. Muscle tension. Headaches. Sleep that’s consistently broken. Heart palpitations that send someone to the ER, only to be told everything looks fine. The emotional piece, the persistent worry and dread, often goes unspoken or gets dismissed as “just getting older.”
That’s part of why research consistently shows anxiety is underdiagnosed in this population. Older adults are more likely to describe their experience in physical terms and less likely to identify it as anxiety. Physicians, focused on managing chronic conditions, can miss it too. The overlap between anxiety symptoms and the side effects of common medications makes diagnosis even harder.
The result is that people suffer longer than they should, and families are left wondering why their loved one seems so unsettled, so withdrawn, or so reluctant to leave the house.
Common signs to watch for include:
- Persistent worry that doesn’t seem tied to any one specific problem
- Irritability or emotional outbursts that feel out of character
- Avoiding activities, appointments, or social situations they once enjoyed
- Restlessness or an inability to sit quietly and relax
- Physical complaints with no clear medical cause
- Increased dependence on family members for reassurance
- Disrupted sleep, either difficulty falling asleep or waking through the night
None of these alone confirms anxiety. But a pattern of several, especially if they’ve appeared or worsened over recent months, is worth a conversation with a doctor.
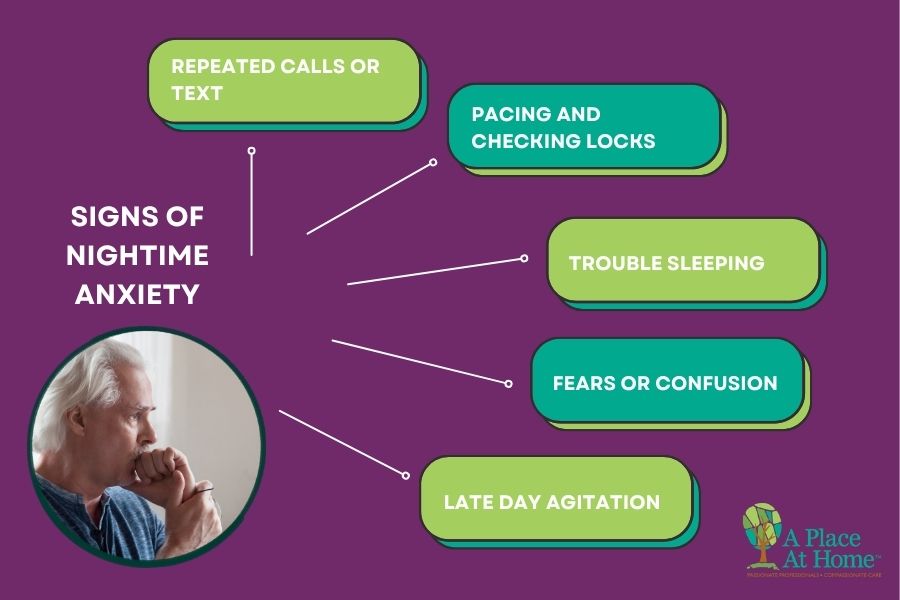
If your loved one’s anxiety tends to get worse in the late afternoon or evening, that pattern has a name. Read our guide on Sundowning and Nighttime Anxiety in the Elderly.
What Actually Causes Severe Anxiety in Older Adults
Late-life anxiety rarely has a single cause. It’s almost always a mix of factors that build on each other over time.
- Chronic illness or ongoing pain: Conditions such as arthritis, heart disease, diabetes, or respiratory disorders can create constant discomfort and uncertainty about health. This ongoing stress can heighten worry and make seniors feel less in control of their bodies and daily lives.
- Medications: Certain prescriptions or combinations of drugs may cause side effects such as restlessness, insomnia, or mood changes. In older adults, who are often managing multiple medications at once, interactions between drugs can sometimes unintentionally worsen anxiety symptoms.
- Emotional loss: The death of a spouse, close friends, or family members can lead to prolonged grief, loneliness, and heightened fear about the future. Similarly, reduced social connections, whether due to retirement, relocation, or limited mobility, can increase isolation and remove important sources of emotional support.
- Loss of independence: Difficulty driving, managing personal care, or completing daily tasks can leave older adults feeling vulnerable or dependent on others. This shift in autonomy can be emotionally challenging and may contribute to persistent worry about safety and dignity.
- Stress from finances and life transitions: Financial stress and major life transitions, such as moving into a new living environment or adjusting to retirement, can further add to uncertainty. Even long-standing financial concerns may feel more pressing in later life when stability and predictability are especially valued.
- History of anxiety: A personal history of anxiety, depression, or trauma can increase the likelihood of experiencing severe anxiety later in life. Past mental health conditions may resurface or become more pronounced when combined with the stresses of aging.

Getting the Right Diagnosis
If you suspect anxiety, the first step is a proper medical evaluation, not a self-diagnosis and certainly not dismissing it as “just how aging feels.”
A primary care physician should assess current medications, run any relevant tests to rule out thyroid conditions, vitamin deficiencies, or cardiac issues that can mimic anxiety, and review the full picture of what the person is experiencing. This step matters because treating anxiety without ruling out medical causes can mean missing something important.
From there, a referral to a mental health professional, a psychologist, psychiatrist, or licensed counselor with experience in geriatric care, allows for a more thorough evaluation. Clinicians use validated tools designed specifically for older adults to assess anxiety severity and identify which type of anxiety disorder may be present.
If your loved one is resistant to the idea of seeing someone, framing it around sleep or stress, rather than mental health, often makes the conversation easier to have.
Treatment Options for Severe Anxiety in the Elderly
Treating severe anxiety in older adults is most effective when approached with a combination of strategies tailored to the individual’s needs, health status, and lifestyle. In many cases, a mix of therapy, medication, and supportive lifestyle changes provides the best results for long-term relief and improved quality of life.
Cognitive Behavioral Therapy (CBT)
CBT is the most thoroughly researched psychological treatment for anxiety in older adults. It works by helping people recognize the thought patterns that fuel anxiety and practice responding differently to them. Over time, worry loses some of its grip.
A 10-year follow-up study published in ScienceDirect found that 70% of older adults treated with CBT were in remission from their primary anxiety diagnosis at the decade mark, compared to 42% in a discussion-based control group. Short-term remission rates from multiple studies range from 40 to 55%. That’s a significant result for a non-medication approach.
CBT doesn’t require a person to be particularly tech-savvy or physically mobile. Research has also confirmed that telephone-delivered and home-based CBT can be just as effective for older adults who can’t easily travel to appointments.
Medications
In some cases, healthcare providers may recommend anti-anxiety medications or antidepressants to help manage severe symptoms. These medications can be effective in reducing persistent worry, panic, or physical symptoms of anxiety when used appropriately.
However, medication use in older adults requires extra caution. Seniors are often more sensitive to side effects, and there is a higher risk of drug interactions due to multiple prescriptions. For this reason, healthcare providers typically start with lower doses and adjust carefully over time.
Ongoing monitoring is essential to ensure the medication is working effectively and not causing unwanted side effects. Regular check-ins with a doctor help maintain safety and allow for adjustments as needed.
Lifestyle and Holistic Approaches
Lifestyle changes can have a powerful impact on managing anxiety, especially when combined with therapy or medication.
- Physical activity: Regular physical activity, such as walking, stretching, or light exercise, helps reduce stress hormones and improve mood.
- Proper nutrition and hydration: Balanced meals can stabilize energy levels and reduce symptoms that may contribute to anxiety, such as fatigue or irritability.
- Improving sleep habits: Establishing a consistent bedtime routine, limiting caffeine, and creating a calm sleep environment can help reduce nighttime anxiety and improve rest.
- Relaxation techniques: Deep breathing exercises, meditation, and mindfulness practices can help seniors regain a sense of control during anxious moments. These tools encourage calmness, lower physical tension, and support emotional balance.
When combined, these treatment options offer a well-rounded approach that addresses both the emotional and physical aspects of severe anxiety, helping older adults feel more secure, supported, and in control of their daily lives.
What Families and Caregivers Can Do
Family members and caregivers play a crucial role in helping older adults manage severe anxiety. While professional treatment is often necessary, consistent support at home can make a significant difference in how well seniors cope with symptoms and maintain stability in their daily lives.
- Providing emotional support and reassurance: Simply listening without judgment and offering calm, steady encouragement can help reduce feelings of fear and uncertainty. Seniors experiencing anxiety often benefit from knowing they are not alone and that someone is there to support them through difficult moments.
- Encouraging healthy daily routines: Establishing structure, such as regular meal times, sleep schedules, light activity, and social interaction, can create a sense of predictability that reduces anxiety. Consistency helps older adults feel more grounded and secure in their environment.
- Assisting with medical management: Keeping track of appointments, helping with transportation, and ensuring medications are taken correctly helps reduce stress and prevent missed treatments or complications that could worsen anxiety symptoms.
- Recognize when additional help is needed: If anxiety symptoms are becoming more severe, interfering with daily functioning, or not improving with current support, it may be time to involve healthcare providers or consider professional care services. Early intervention can prevent symptoms from escalating and improve overall outcomes.
- Avoiding the invalidation of symptoms: Statements like “just relax” or “you’re fine” may be well-intentioned but can make seniors feel misunderstood or dismissed. Instead, acknowledging their feelings and responding with empathy helps build trust and encourages open communication.
When caregivers combine patience, structure, and emotional understanding, they create a supportive environment that plays a powerful role in helping older adults better manage anxiety and improve their overall quality of life.
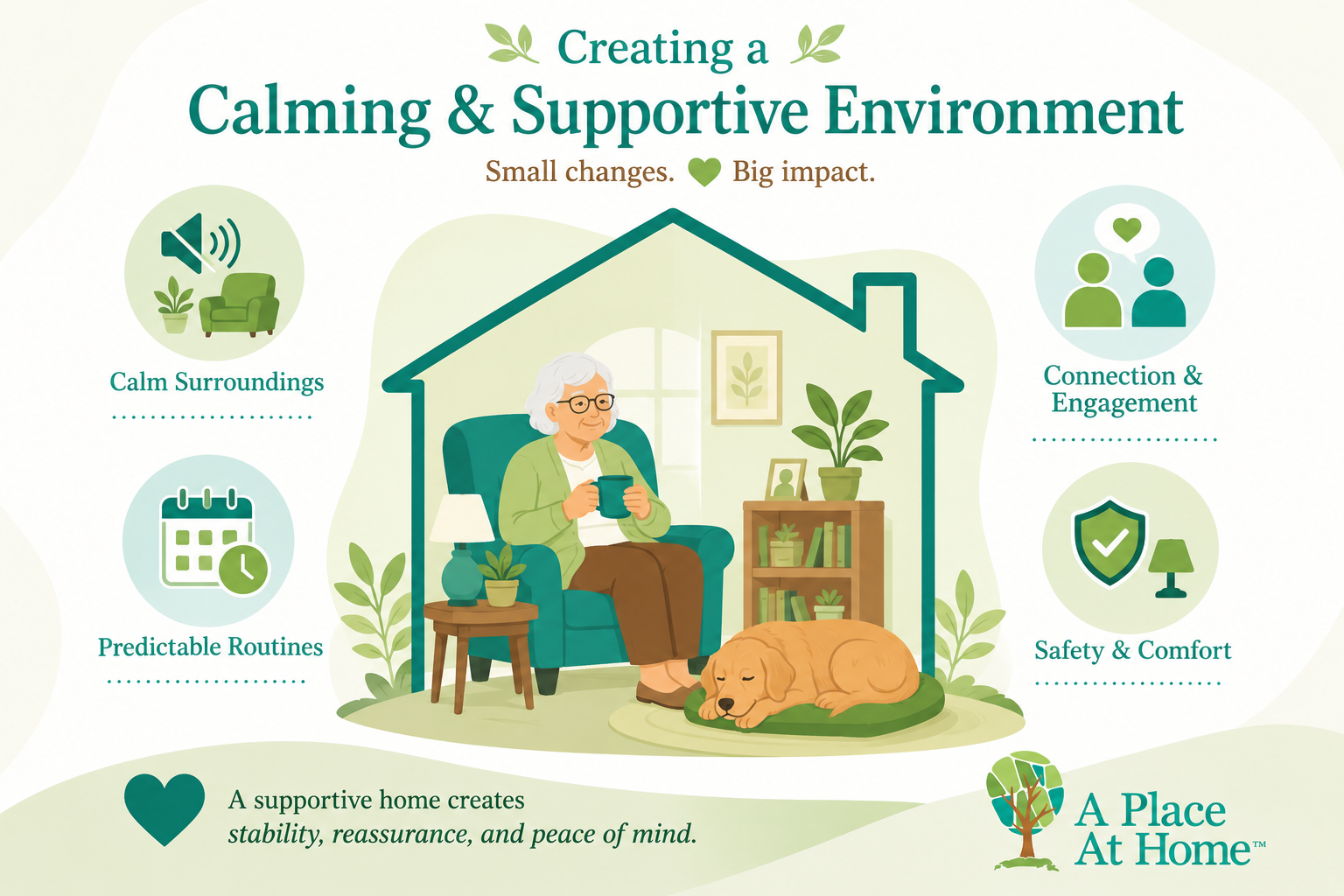
Creating a Calming and Supportive Environment
A supportive home environment can play a major role in reducing anxiety and helping older adults feel more secure in their daily lives. Small, intentional changes in surroundings and routines can significantly lower stress levels and promote a greater sense of calm and stability.
- Reducing stress triggers at home: This may include minimizing loud noises, limiting clutter, and creating quiet spaces where the individual can relax without distraction. A calm, organized environment can help prevent feelings of overwhelm and make daily living feel more manageable.
- Establishing predictable routines: Consistent schedules for meals, sleep, medication, and daily activities help create structure and reduce uncertainty, one of the common contributors to anxiety. When seniors know what to expect each day, they often feel more in control and less anxious.
- Social interaction and engagement: Regular visits with family, participation in community activities, or even simple phone calls can help reduce isolation and provide meaningful emotional connection. Staying socially active has been shown to improve mood and reduce feelings of worry and loneliness.
- Safety and comfort considerations: Ensuring that the home is free of hazards, well-lit, and easy to navigate can help reduce fear of accidents or injury. Comfort items such as familiar furniture, personal belongings, or calming spaces can also provide reassurance and emotional grounding.
When these elements are combined, the home becomes more than just a living space, it becomes a place of stability, reassurance, and emotional support that can significantly ease symptoms of severe anxiety in older adults.
When to Consider Professional In-Home Care Support
There may come a point when family support alone is not enough to fully meet the needs of an older adult struggling with severe anxiety. Recognizing when additional help is needed is an important step in ensuring safety, comfort, and overall well-being.
- Anxiety begins to interfere with daily functioning: This may include difficulty managing personal care, preparing meals, taking medications correctly, or leaving the home due to fear or excessive worry. Increased forgetfulness, frequent distress, or withdrawal from normal activities can also signal that extra support is needed.
- Professional caregivers can provide meaningful benefits: Trained caregivers offer both practical assistance and consistent emotional reassurance, helping seniors feel more secure throughout the day. Their presence can also ease the burden on family members who may be balancing caregiving with other responsibilities.
- Reducing isolation and stress: Having a trusted caregiver present can provide companionship, encourage conversation, and promote engagement in daily activities. This regular interaction helps combat loneliness, which is often a major contributor to anxiety in older adults.
- Physical and well-being support services: These may involve assistance with personal hygiene, meal preparation, medication reminders, light housekeeping, mobility support, and transportation to appointments. Together, these services help create a safer, more structured environment that promotes stability and reduces anxiety triggers.
Senior Home Care from A Place At Home – Weston
Severe anxiety in older adults is a real and treatable condition, not simply an expected part of aging. With the right combination of medical care, emotional support, and consistent daily structure, many seniors can experience significant relief and regain a greater sense of calm and confidence in their everyday lives.
What matters most is early recognition and compassionate intervention. Whether it’s through therapy, medication, lifestyle changes, or supportive caregiving, addressing anxiety holistically can make a meaningful difference in both mental and physical well-being. Families and caregivers play a vital role in this process by offering patience, understanding, and encouragement throughout the journey.
In some cases, additional support becomes necessary to ensure safety, reduce isolation, and improve quality of life. Professional in-home care can provide that extra layer of consistency and reassurance that helps seniors feel more secure and supported in their own homes.
If your loved one is struggling with anxiety or needs extra day-to-day support, compassionate help is available. A Place At Home – Weston offers personalized senior care services designed to support both emotional and physical well-being, helping older adults remain safe, comfortable, and engaged at home.
Call us at (954) 335-9284 to learn more about our senior care services in Weston, FL and the surrounding areas of Broward County.
Senior Anxiety FAQs
What is the best anti-anxiety medication for elderly?
There is no single “best” anti-anxiety medication for older adults, because treatment must be individualized. In many cases, doctors may prescribe selective serotonin reuptake inhibitors (SSRIs) such as sertraline or escitalopram as a first-line option due to their generally safer profile in seniors. However, response, side effects, existing medical conditions, and other medications all influence the choice. Because older adults are more sensitive to side effects, clinicians typically start with low doses and monitor closely.
What is the most common cause of anxiety in the elderly?
The most common causes of anxiety in older adults are usually a combination of factors rather than one single trigger. These often include chronic health conditions, chronic pain, loss of independence, grief after losing loved ones, social isolation, and major life transitions such as retirement or relocation. A history of anxiety earlier in life can also increase the likelihood of symptoms returning or worsening later on.
What are symptoms of anxiety in the elderly?
Anxiety in older adults can appear in emotional, physical, and behavioral forms. Common symptoms include:
- Excessive worry or fear that is difficult to control
- Irritability or restlessness
- Fatigue and low energy
- Muscle tension or headaches
- Sleep disturbances (difficulty falling or staying asleep)
- Heart palpitations or shortness of breath
- Avoidance of social activities or responsibilities
- Increased withdrawal or isolation
- Difficulty concentrating or feeling “on edge”
These symptoms can sometimes overlap with other medical conditions, which is why proper evaluation is important.
Does social anxiety get worse with age?
Social anxiety does not necessarily worsen with age for everyone, but it can become more noticeable or limiting in some older adults. Factors such as reduced mobility, hearing or vision changes, loss of peers, or increased health concerns may make social situations feel more stressful or exhausting. On the other hand, some individuals experience improvement over time as they adapt coping strategies and prioritize smaller, more comfortable social circles.
What medication is used for panic attacks in the elderly?
Panic attacks in older adults are typically treated cautiously. SSRIs (such as sertraline or citalopram) are often used for long-term prevention of panic symptoms. In short-term or acute situations, doctors may sometimes prescribe benzodiazepines, but these are generally used with great care in the elderly due to risks such as sedation, falls, and dependence. Treatment decisions depend on overall health, other medications, and the severity of symptoms, and should always be managed by a healthcare professional.



 If your loved one is waking frequently or struggling with disrupted sleep patterns, you may also find this helpful:
If your loved one is waking frequently or struggling with disrupted sleep patterns, you may also find this helpful: